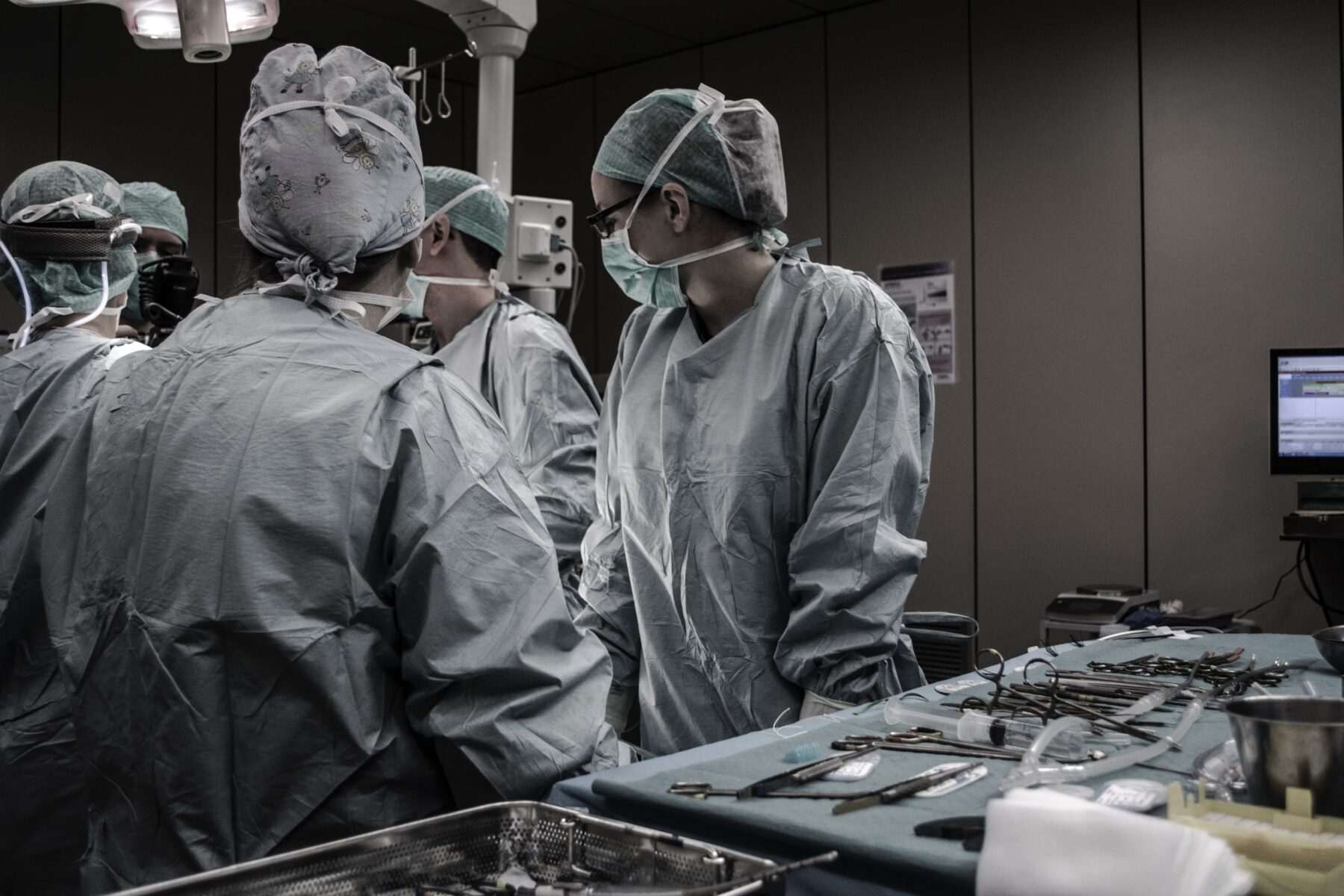
Minimizing infections when reprocessing endoscopy equipment
Endoscopic procedures involve a flexible or rigid tube with a light and camera attached to it which is inserted into an organ cavity.
This invasive imaging technique is sometimes combined with specific surgical procedures. Endoscopes fall into categories based on the area of the body that they investigate. The Food and Drug Administration states that in the U.S., duodenoscopes are used in more than 500,000 endoscopic procedures annually. The advancement in these medical devices for the treatment of gastrointestinal diseases is evident.
However, there is a link between infections and inadequately cleaned endoscopes, specifically duodenoscopes due to their complex design, which remains unsettling among many health care organizations. According to the Centers for Disease Control and Prevention, outbreaks of bacterial infections are associated with endoscopes being improperly reprocessed. Due to duodenoscopes containing many small working parts over other types of endoscopes, the instrument can be more difficult to clean and disinfect. If not thoroughly cleaned and disinfected after each use, tissue or fluid from one patient can remain in the device when it is used on a subsequent patient, causing an infection to be acquired via patient-to-patient or environment-to-patient.
Failing to clean endoscopes correctly can also result in the instrument channels becoming blocked, leading to inadequate functioning. After an agency-led expert panel meeting in 2015 regarding concerns with endoscope reprocessing, the FDA published a guidance that provides a detailed list of reprocessing measures, in addition to meticulously adhering to the manufacturer instructions for health care facilities to follow. The purpose of this guidance is for health care facilities to take one or more additional steps to further reduce the risk of infection, maximize patient safety and increase the safe handling of these medical devices. The FDA encourages health care facilities to understand the importance of their role in reprocessing the device as well as maintaining proficiency in performing these reprocessing tasks.
As a supplement to the manufacturer reprocessing instructions and the recent FDA guidance, health care facilities should consider the following six steps when assessing the adequacy of reprocessing common endoscopy devices:
Staff training
Ensuring personnel performing the endoscope reprocessing procedures have received appropriate training with competency verification will enhance patient safety. Training should be introduced at the initiation of employee duties, and then reevaluated on an annual basis, anytime a breach is identified or a new technique or equipment is introduced. When developing an endoscope reprocessing education and training program, there may be different needs for the various types of personnel who are cleaning and reprocessing endoscopes.
Therefore, materials should be established for the unique role each staff member plays. For example, training for a staff member who performs pre-cleaning and transports the endoscope to a central reprocessing area will be very different than a staff member who works in the reprocessing areas. Competency verification should include direct observation in addition to other assessments such as written tests. With innovative, cloud-based technology, there are some new programs available to health care facilities that will reduce the need for meetings and align their vendors and staff around relevant training topics. Health care facilities should require all personnel responsible for reprocessing endoscopes to receive proper certification, specifically in line with the manufacturer of each device.
Manual cleaning
It is vital to clean endoscopes manually in a room dedicated to the purpose of removing the organic debris and microorganisms that may be present. Personnel responsible for reprocessing should flush the air/water channel to expel any blood, mucus or other debris. To clean the outer surface of the endoscope thoroughly, all valves should be removed and cleaned separately with a soft brush. It is important to pay particular attention to the control section, angulation controls, distal end and the bridge mechanism of duodenoscopes. After removing the instrument from the electrical equipment, fully immerse and wash the suction channel in warm soapy water with a flexible brush. The used brushes should then be cleaned thoroughly by putting them through an ultrasonic cleaner before they are sterilized and repackaged. Always refer to the manufacturer’s recommendations specific to each component.
Surveillance culturing
Health care facilities may perform microbiologic culturing, which involves sampling endoscope channels to identify any bacterial contamination that may be present on the scope after reprocessing. International guidelines have recommended intervals ranging from every four weeks to annually. Although numerous health care facilities have successfully implemented routine or periodic microbiological culturing, the CDC encourages that additional data and validation testing is needed to demonstrate the robust methodology and reliable culturing results before health care facilities can incorporate it as a best practice.
Competency
To ensure that manual cleaning is performed consistently and accurately, the FDA panel recommends strengthening competency training for reprocessing staff in health care facility reprocessing units and incorporating human factors testing when developing reprocessing instructions. Additionally, to prevent the risk of infection, single-use or autoclavable accessories should be used wherever possible. Do not reuse accessories labeled for single use.
Recordkeeping
Health care facilities should develop procedures and responsibilities for tracking the useful life of endoscopes and accessory equipment, including equipment and supplies for reprocessing. These procedures should address specification evaluation, scheduled maintenance and removal of equipment from use. Identify all endoscopes, endoscope accessories and endoscope reprocessing equipment used in your facility, including manufacturer, models, serial numbers or hospital-specific equipment tag numbers and unique device identifiers (UDIs). It is important to also include the location within the facility where the equipment is reprocessed and stored, and the status or maintenance schedule of the device.
Infection preventionists play an important role in endoscopy leadership and quality reporting to further reduce the risk of infection and increase the safety of endoscopes. It is critical that health care organizations include endoscope-related infections in surveillance activities in the event that an environment-to-patient infection is acquired, also referred to as a health care associated infection (HAI). Although conducting surveillance for HAIs is part of every infection preventionist’s job, there is not a standard definition set for determining if a patient acquired an infection from an endoscope. Therefore, it is critical to examine all aspects of the endoscope reprocessing programs to ensure that staff are meticulously adhering to the cleaning and reprocess instructions.
Imagine this scenario: an endoscopy unit at a major hospital is in the midst of a large construction renovation project. The endoscopy equipment and accessories were just cleaned and sterilized by the appropriate hospital staff for use on the next patient. Various construction vendors carrying potentially harmful debris unknowingly on their shoes and clothing are walking in and out of the area where these sterilized devices are being stored. If even the smallest amount of dust or other bacteria-laden debris becomes airborne and falls onto sterilized endoscopy equipment that then enters a patient, specifically an immunocompromised patient, the result could be deadly.
Additionally, some ventilation systems in the endoscopy units were not sealed securely, causing bacteria from the construction site to enter the clean areas in the facility. Due to poor surveillance and record keeping, this health care facility’s role in HAI prevention could be in jeopardy. Although this scenario is not a direct result of improper endoscopy reprocessing, it is a very plausible and preventable situation that should be considered.
When the FDA investigated other cases concerning endoscopy reprocessing issues, the investigators identified the same source of transmission: a specialized endoscope, threaded down the throat of a half-million patients a year to treat gallstones, cancers and other disorders of the digestive system. They found that the duodenoscope devices accumulated bacterium that was not fully removed by conventional cleaning techniques, causing an infection to pass from patient to patient. This bacterium is known as Carbapenem-Resistant Enterobacteriaceae (CRE), an antibiotic-resistant superbug that can kill up to 40 percent of the people it infects.
Endoscope cleaning machines can cost roughly $30,000 to $50,000 and typically take about 30 minutes to wash with disinfectant following some manual cleaning. The FDA estimates that about 1,000 hospitals and clinics nationally rely on the manufacturer’s equipment to prepare reusable endoscopes for the next patient. Most hospitals that do these procedures are not even looking for this problem, or they may not be aware. Even when the devices are cleaned strictly in accordance with manufacturer and FDA-approved guidelines, there is still a great risk of infections being transmitted.
While the FDA is studying the problem and working with manufacturers to determine whether new cleaning protocols should be mandated or the endoscopes should be redesigned entirely, health care facilities must act now to do what they can to maintain patient safety and prevent exposure to endoscope-related infections. Ensuring a safe and reliable endoscope program requires a multidisciplinary approach and is truly a team effort in order for it to be successful.